Endometriosis is a common disease that can affect the quality of life, and in some cases, the fertility of many women. According to the World Health Organization (WHO), it affects approximately 10% of women of reproductive age1. Furthermore, it is estimated that between 25% and 50% of women with infertility have endometriosis1,2.
One of the main challenges of this pathology is its diagnosis, as it can present with a wide range of symptoms: from asymptomatic forms to conditions that significantly impact daily life.
What is endometriosis?
Endometriosis is a disease characterized by the presence of endometrial tissue outside the uterus.
The endometrium is the tissue that forms the inner lining of the uterus, which sheds during each cycle, resulting in menstruation. In women with endometriosis, this tissue can implant in other areas, such as:
- The ovaries
- The fallopian tubes
- The bowel
- The peritoneum
- Other locations outside the pelvic cavity.
Depending on its location, two types of endometriosis can be distinguished:
- Internal endometriosis, when it affects structures within the pelvic cavity, such as the ovaries or the myometrium.
- External endometriosis, when it appears in organs outside the pelvic area.
Additionally, it can present in different forms:
- Disseminated implants
- Nodules
- Endometriomas (ovarian cysts)
- Adherences.
Symptoms of endometriosis: how to identify them
The symptoms of endometriosis are highly variable and do not always correlate directly with the extent of the disease. However, there are a series of signs that appear more frequently and are worth knowing and identifying.
Pelvic pain or cramping outside of menstruation
Pain in the lower abdomen outside of the menstrual period is one of the common symptoms. In some cases, it manifests as ovarian pain or in the form of cramps, and it may be related to chronic inflammatory processes, such as endometriosis.
Severe menstrual pain
Severe menstrual pain or dysmenorrhea is one of the most characteristic symptoms of endometriosis. When menstrual pain interferes with daily activities, it should never be considered normal and requires medical evaluation.
Pain during or after sexual intercourse
Pain during sexual intercourse (dyspareunia) is frequent, especially in deeper forms of the disease. This pain can appear during intercourse or in the hours following it.
Intermenstrual bleeding
Bleeding outside of the menstrual period, while not necessarily pathological, can also be another warning sign. When it is recurrent and not accompanied by a physiological process that explains it (such as ovulation), it requires clinical evaluation.
Digestive and urinary symptoms
When endometriosis affects nearby organs, symptoms such as painful bowel movements, diarrhea or constipation, and an increased frequency of urination may occur. These symptoms typically intensify during menstruation.
It is important to bear in mind that no single symptom on its own is diagnostic of endometriosis. However, their presence, especially if persistent, justifies a medical evaluation.
Endometriosis and fertility
Endometriosis is one of the leading causes of female infertility. It can affect fertility through various mechanisms, such as altering ovarian function, causing chronic inflammation in the pelvic environment, or making embryo implantation difficult. For this reason, when there are difficulties in achieving a pregnancy, it is important to rule out this pathology.
How is it diagnosed?
The diagnosis of endometriosis is based on a combination of medical history, physical examination, and imaging tests. The most commonly used are:
- Gynecological examination
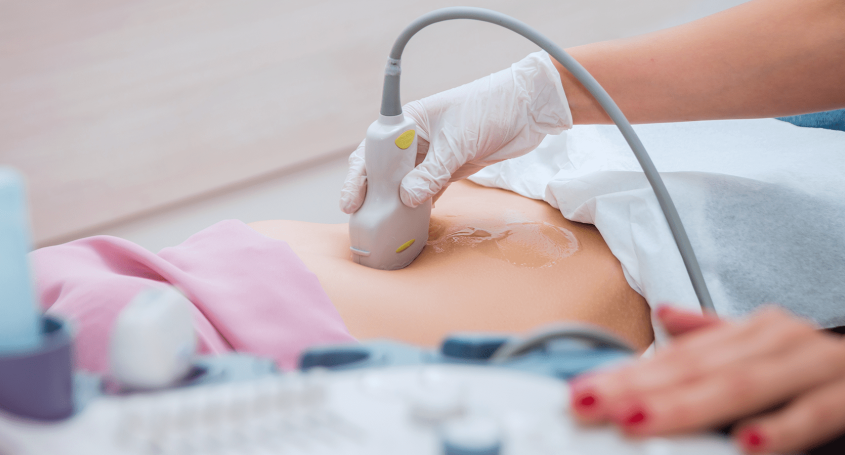
- Transvaginal ultrasound
- Magnetic resonance imaging (MRI)
- Laparoscopy, in some more complex cases.
Currently, non-invasive techniques are prioritized, reserving laparoscopy for very specific situations.
Treatment options for endometriosis
The treatment of endometriosis depends on multiple factors, such as the intensity of the symptoms, the location of the lesions, the patient's age, and their reproductive desires.
- Pain management, using analgesics and anti-inflammatory drugs.
- Hormonal treatment, through contraceptives, progestogens, or GnRH analogues.
- Surgical treatment, aimed at removing the lesions.
- Assisted reproduction techniques, in cases where endometriosis affects fertility.
How do we approach endometriosis at Barcelona IVF?
At Barcelona IVF , we approach endometriosis from an integral and personalized perspective. Our team evaluates each case individually, taking into account the degree of involvement of the disease and the desires of each patient, in order to offer a tailored and effective treatment.
1. World Health Organization. Endometriosis [Internet]. Geneva: World Health Organization; 2023 [cited 2026 Mar 27]. Available from: https://www.who.int/news-room/fact-sheets/detail/endometriosis
2. ESHRE Guideline Group; Becker CM, Bokor A, Heikinheimo O, Horne A, Jansen F, Kiesel L, et al. ESHRE guideline: endometriosis. Hum Reprod Open. 2022;2022(2):hoac009. doi:10.1093/hropen/hoac009