Artificial insemination Spain

What are the steps of the process?
Artificial insemination consists of three main steps:


How is the treatment performed?
Find out everything you need to know.
General information
Artificial insemination is recommended for cases in which the woman is not over the age of 38, although this could be extended when it is not a sterility problem. Indications for artificial insemination are:
- No partner or female partner that requires the use donor sperm
- When the cause of sterility is unknown despite having performed the basic fertility evaluation
- When there is a mild male factor that can improve with sperm preparation in the laboratory
- When there is a severe male factor that recommends the use of donor sperm
- When there are ovulation abnormalities
- When a couple has difficulty having sexual intercourse
In all these cases, it is recommended that you go to an “artificial insemination clinic” specialising in assisted reproduction to achieve a pregnancy.
The recommended tests for performing artificial insemination are:
- Hormone test to examine the ovarian reserve. The Anti-Müllerian Hormone (AMH) value can be determined at any time during the cycle, and the FSH and Estradiol value on day 3 of the cycle.
- Semen analysis with motile sperm recovery (MSR) test to evaluate whether the partner’s sample is of sufficient quality to perform an insemination.
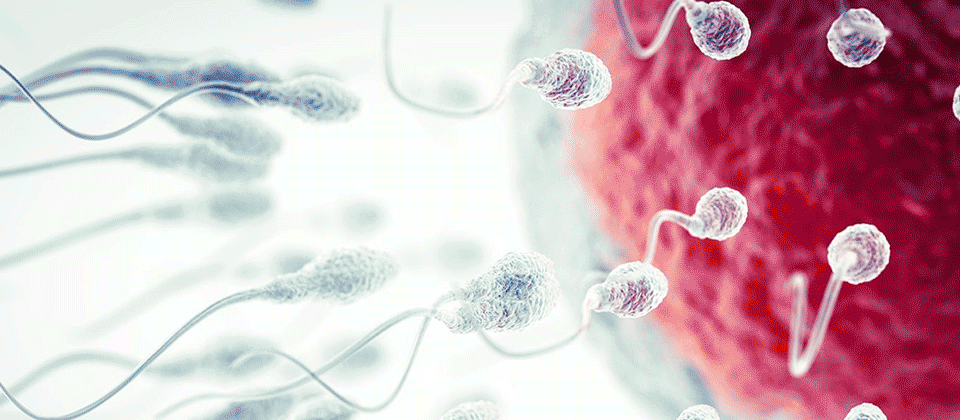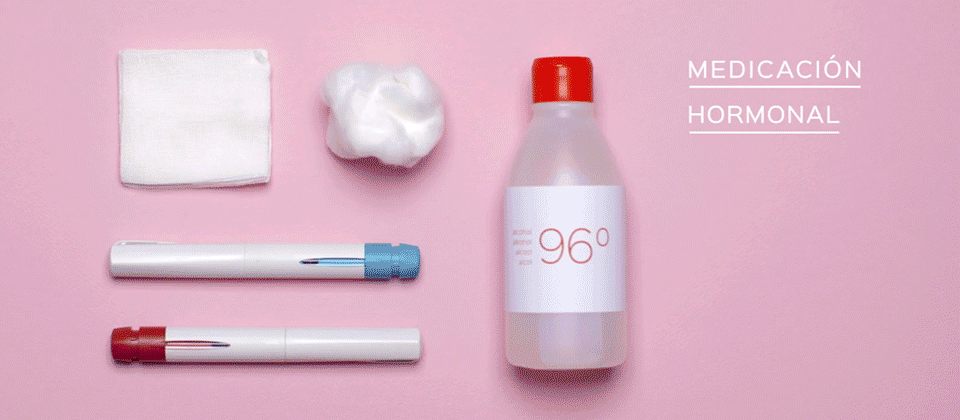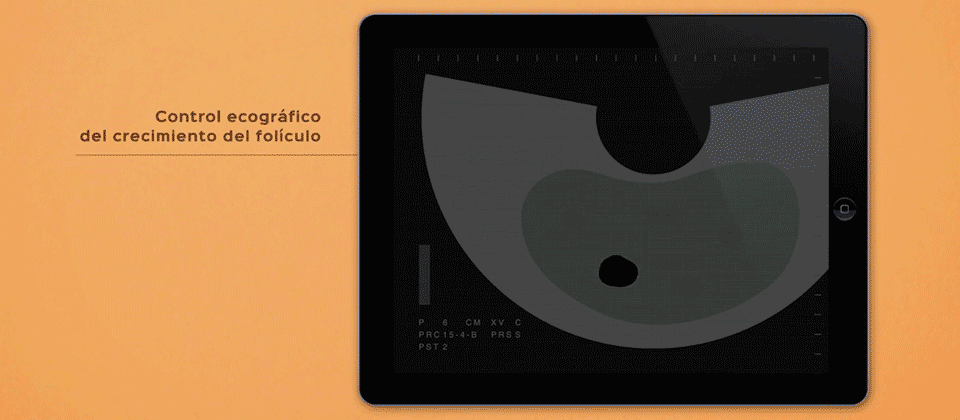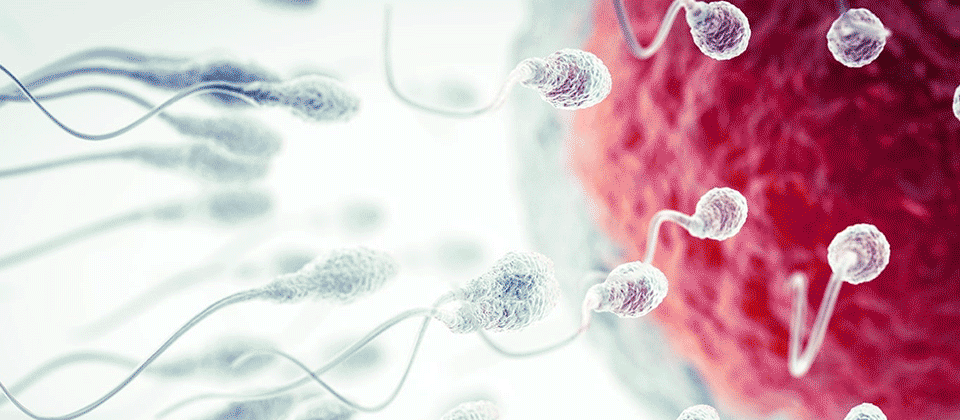
- Gynaecological ultrasound to rule out uterine and ovarian diseases. It is also used to evaluate the ovarian reserve by antral follicle count.
- Hysterosalpingography to evaluate tubal permeability. It consists of a contrast injection into the uterine neck while x-rays are being performed.
- Serologies to rule out the presence of transmissible infectious diseases.
The success rates for inseminations remain stable during the three first attempts. If no pregnancy is achieved after 3 inseminations, we recommend trying a different and more effective treatment.
Ovarian stimulation and gynaecological tests

Sperm collection and preparation
Care after artificial insemination

Positive results
The rates for pregnancy achieved with artificial insemination depend on the patient’s age. These rates are similar to those a non-sterile couple have during a natural cycle.
Partner sperm
Donor sperm
What does artificial insemination treatment include?
Artificial insemination fertility treatment includes:
- Medical appointments
- Insemination
- Ultrasound scans during the cycle
- B-hCG
- Hormone tests during the cycle